Last weekend, a finance CEO shipped an open-source MRI viewer because his six-year-old daughter has brain cancer and he got tired of comparing her scans by hand.
Here's the thing. The tool he built in a weekend doesn't exist commercially. Not from Siemens or GE or from any of the $250M+ AI imaging startups. The entire medical imaging market, $3.3 billion and growing, is optimized for looking at one scan at a time. Nobody built for the question cancer patients ask most: Is it growing?
That's a venture-scale gap. And this is the case for filling it.
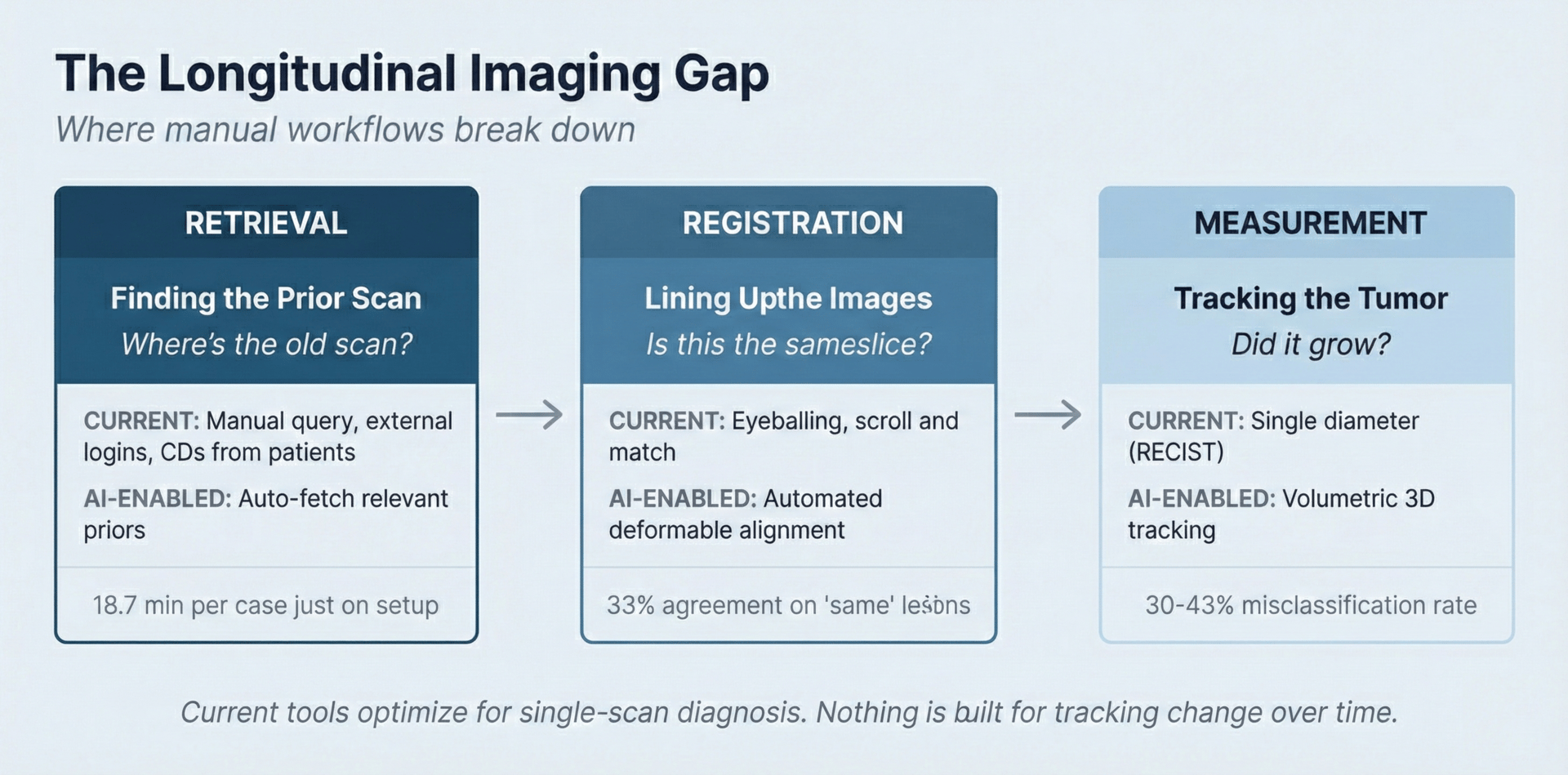
Every few months, a patient gets scanned. The radiologist opens the new MRI, pulls up the old one from the archive, scrolls through hundreds of slices to find the same spot, eyeballs the rotation, adjusts for contrast differences, and measures with digital calipers. They're trying to match the exact angle used months earlier by a different doctor.
This is the state of the art.
The global standard for measuring tumors is called RECIST 1.1. It was created in 2000 and updated in 2009. It measures the longest width of up to five tumors and calls it a day.
The assumption: tumors are basically round, and if the width changes, the volume changes too. But that's often wrong. A tumor can grow 40% in volume while only showing a 10% increase in width. That's below the threshold for "getting worse." So the patient looks stable on paper while their cancer keeps growing. Doctors call this pseudostability. It's a fancy word for "we missed it."
How much do tumor measurements vary between doctors?
±22%
Enough to flip a "stable" diagnosis to "progressing."
In one study, three radiologists agreed on the "five largest" tumors only 33% of the time. Another found that fewer than 10% of patients had the same tumors selected by different reviewers.
What does this add up to? Between 30-43% of tumors get misclassified. Radiologists spend an average of 18.7 minutes per cancer case just on comparison.
For kids with cancer, it's even harder. The rules designed for adults don't work for pediatric brain tumors. New criteria called RAPNO were developed, but studies still show up to 8% of cases get staged wrong in clinical trials.
Here's the real problem. In cancer care, the important thing isn't what the scan shows today. It's how today compares to last time. The signal is in the change. And almost nothing is built to measure change.
Siqi Chen built MiraViewer: a free tool that loads MRI files, lines up scans from different dates automatically, lets you mark tumors, and shows them side by side. It runs directly in your browser.
He built it because his daughter was diagnosed with an adamantinomatous craniopharyngioma; an extremely rare pediatric brain tumor. His family needs to consistently track her scans.
"We got pretty good at this. But it shouldn't be this hard."
— Siqi Chen
So what would a real company look like?
The product: take what MiraViewer does and make it clinical-grade. Get FDA clearance. Add volumetric tracking that measures the whole 3D tumor, not just one slice. Build reports that plug into hospital systems. Handle the hard cases: brains after surgery, scans from different machines, kids whose anatomy looks nothing like adults.
The technical edge: AI that knows the difference between "the images don't line up right" and "the tumor actually grew." Software that adjusts for different MRI machines automatically. Models trained specifically on childhood cancers.
The path to market: pure open-source companies haven't worked in healthcare. Hospital sales go through IT and procurement, not developers downloading things from GitHub. The smarter play looks like Livongo: start with tools for patients and caregivers, build a community, then flip to selling to hospitals and cancer centers.
The comparisons: Cleerly proved you can build a company around tracking disease over time. They measure heart plaque and raised $106M in late 2024. Rad AI raised $60M in early 2025 for automating radiology reports. Cortechs.ai has FDA clearance for measuring brain volume changes. None of them do what MiraViewer does.
The medical imaging software market is about $3.3 billion and growing 7-8% per year. The AI piece is smaller but moving faster: $576M in 2022, expected to pass $2B by 2028.
Healthcare AI investment in 2025
$10.7B
Up 24% from the year before.
But investors are getting pickier. They want platforms that stick, not one-trick tools. So who would want to fund something like this?

What gets you funded at seed? A working prototype, a regulatory plan, and pilots with academic hospitals. For a Series A, you need FDA progress, real clinical data, integration with existing hospital systems, and proof that you save time or money.
The open-source question is tricky. In developer tools, giving away software and charging for extras works great. But healthcare sales go through procurement departments, not individual users. Open-source can help you get noticed, but it's not a business model by itself.
Siqi’s daughter was diagnosed last September. Her family did something extraordinary. They put together a private research team, raised $1.4M, and got her into an experimental treatment program through UCSF Benioff Children's Hospital and the University of Colorado.
The tumor responded to a combination of tocilizumab and Avastin. It's working. But she’ll still needs brain MRIs every few months. For years. Maybe for the rest of her life.
The scan comparison problem Siqi solved in a weekend is the same problem facing thousands of cancer families, and the doctors treating them.
The manual process exists because the big imaging companies optimized for emergencies, not long-term tracking. The venture opportunity exists because nobody bothered to fix it.
This is a pattern worth watching. Caregivers building tools that should already exist. PocketHealth lets patients own their imaging records. Ezra is building end-to-end MRI screening. Cancergraph lets patients track symptoms alongside their disease. The best healthcare tools are increasingly built by the patients.
MiraViewer might become a company. It might get picked up by an existing platform. It might stay what it is now: a gift to other families going through the same thing.
But the gap it exposes is real.
The first wave of imaging AI was about emergencies. Stroke alerts. Bleeding detection. The "stat" diagnosis. The second wave is about tracking. Measuring. Watching things change over time.
Whoever figures out the "tracking over time" problem owns a critical piece of cancer care. The science is broken. The market is wide open. The case is here.
Now can someone build it?
If this was useful, forward it to someone building in biotech. More stories like this every week at Thinking Folds.